Chronic disease drives most of Medicare’s spending and much of the daily complexity that provider groups manage. Yet for decades, traditional fee-for-service has made it difficult to deliver the kind of longitudinal, proactive care that clinicians know leads to better outcomes.
With the introduction of the ACCESS Model, CMS is signaling a meaningful shift. ACCESS is a long-term, outcomes-based framework designed to support modern, technology-enabled chronic care in Traditional Medicare. Many details are still forthcoming, but the direction is clear: Medicare is moving toward a tech-forward model that rewards improvement, continuity, and patient-centered management of chronic conditions.
What ACCESS Is, and Why It Matters
ACCESS is a 10-year voluntary model launching in 2026 that centers on chronic conditions affecting a majority of Medicare beneficiaries, including hypertension, diabetes, chronic musculoskeletal pain, and behavioral health conditions such as depression and anxiety.
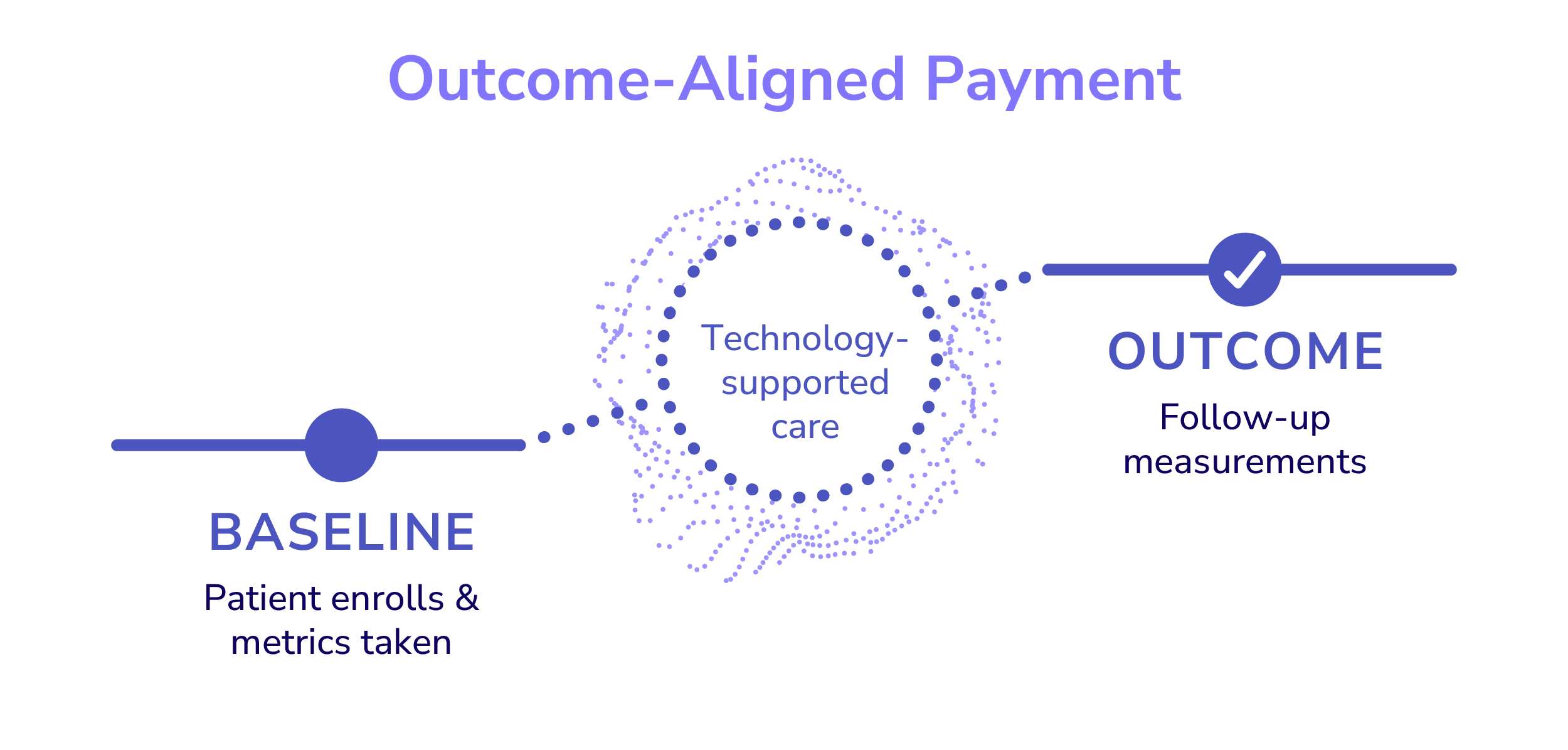
The model’s central innovation is the use of Outcome-Aligned Payments (OAPs): recurring payments tied to clinical and patient-reported outcomes measured against each patient’s own baseline. Measures vary by condition and reflect meaningful indicators of improvement, stability, or deterioration.
ACCESS also explicitly embraces technology-supported care. Remote monitoring, virtual visits, asynchronous communication, and digital therapeutics can all be incorporated into patients’ care pathways. The model recognizes that much of chronic care management occurs between visits and seeks to create a payment structure that supports that reality.
Another important distinction: ACCESS has no claims-based patient alignment. Patients must actively enroll or be referred in, creating new opportunities for providers to engage patients directly.
For provider groups of all sizes, even those not currently in risk arrangements, ACCESS offers a new, flexible pathway into value-based care, grounded in outcomes rather than service volume.
Why ACCESS Should Be on Providers’ Radar
ACCESS has the potential to reshape how chronic care is supported across Traditional Medicare:
- A predictable payment mechanism for longitudinal, technology-enabled care. Providers can be reimbursed for work that has historically lacked a stable payment structure.
- Support for proactive care between visits. ACCESS encourages clinicians to use digital tools to close gaps, adjust treatment plans, and guide patients more consistently.
- Alignment with patient expectations. Remote-friendly and convenient modalities meet patients where they are and reduce friction in managing chronic conditions.
- A no-risk opportunity to test tech-enabled chronic-care approaches. Payments do not accrue against ACO benchmarks for the first 1.5 years, allowing Providers to pilot and refine new workflows without risking their performance in programs like MSSP or ACO REACH.
Key Differences Between ACCESS and Other Models
ACCESS introduces two notable shifts that distinguish it from other Medicare innovation models and shape how providers will participate.
First, ACCESS is built on patient-specific baselines, rather than population benchmarks. Instead of comparing performance against regional or historical norms, as in MSSP or ACO REACH, ACCESS evaluates improvement relative to each individual patient’s starting point. This design rewards consistent, technology-enabled engagement that helps patients make measurable progress over time. Establishing a reliable baseline, supporting patients between visits, and trending outcomes in a low-burden way become central to success.
Second, ACCESS introduces a different enrollment motion. The model does not use claims-based attribution; patients must actively enroll or be referred in. While this differs from the attribution used in other models, it creates opportunities for more intentional conversations with patients about their goals and the benefits of proactive, tech-enabled chronic care.
Unknowns Providers Should Be Aware Of
Several important details of ACCESS are still forthcoming:
- Payment amounts for OAPs have not yet been released, leaving open questions about the magnitude of financial opportunity.
- Performance thresholds and detailed outcome specifications are still under development.
- Data and reporting expectations may evolve as CMS continues to refine the model.

Most of these details represent temporary uncertainties that should be clarified when the RFA is released in the coming weeks. In the interim, establishing the core capabilities ACCESS requires—interoperability, remote patient engagement, and outcome tracking—remains a sound operational strategy regardless of the final model parameters.
What Providers Can Do Now
There are practical, incremental steps organizations can take today to prepare:
- Audit chronic-condition prevalence across your patient panel.
- Map existing digital capabilities, including telehealth, asynchronous communication, remote monitoring, and EHR integration.
- Identify opportunities for automation to streamline routine tasks and surface actionable insights.
- Pilot focused workflows: for example, a hypertension management pathway or diabetes follow-up protocol.
- Monitor CMS updates closely as the model specification evolves.
Each of these steps builds operational strength that benefits patients now and positions providers for early success when ACCESS launches.
How Pearl Health Can Help
As CMS continues to introduce new innovation models, determining the right path can be complex. Pearl acts as a strategic advisor to help provider groups navigate these changes and identify the best opportunities for their practice.
We help organizations assess their data and patient populations to understand where they can drive the most value. By establishing a flexible foundation for outcomes-focused care today, providers gain the agility to evaluate emerging options, so they can participate in models like ACCESS with confidence when opportunities arise.
Conclusion: A Moment of Real Opportunity for Provider-Led Innovation
ACCESS represents another meaningful step toward a future where Medicare rewards outcomes rather than volume. It aligns Medicare with the direction the best healthcare organizations have rapidly been embracing: proactive, connected, patient-centered care supported by modern technology.
The shift toward outcomes-driven, technology-enabled chronic care is accelerating. ACCESS is a clear signal of where Medicare is heading, and an invitation for providers to help shape what comes next.


