The Hidden Problem in Post-Acute Care
Skilled Nursing Facilities (SNFs) play an important role in helping patients get back on their feet after a hospital stay, providing critical therapies and rehabilitation when a patient needs more support than they could get at home.
However, current Medicare payment structures may unintentionally encourage longer-than-necessary stays. This isn't just a policy issue, but a patient care issue — it can lead to unnecessarily long stays away from home, medical risks, and loss of control for patients.
One Pearl primary care physician in New York put it bluntly:
"Some SNFs manipulate patient stays to maximize Medicare reimbursements. For example, they might falsely claim a patient has a wound requiring extended care just to keep them longer."1
These policy misalignments are costly. They drive unnecessary spending across the system and may reduce trust in the healthcare institutions meant to protect and serve patients.
How Medicare’s SNF Payment System Enables Overstays
Under Medicare Part A, the cost of care in a SNF is partially covered for up to 100 days for each benefit period. Whereas the first 20 days are fully covered, days 21 through 100 place some responsibility on patients via a daily coinsurance payment.2 Some SNFs strategically time patient discharges around that 20-day mark to ensure they receive the maximum reimbursement possible from Medicare. Others look for reasons to keep patients longer and will bill for the daily charges that begin after day 20. A 2018 study found that some providers make discharge decisions based on financial incentives, not necessarily based on what patients need.3
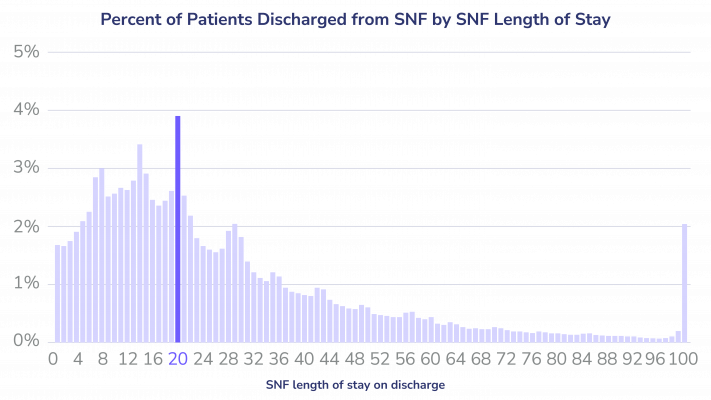
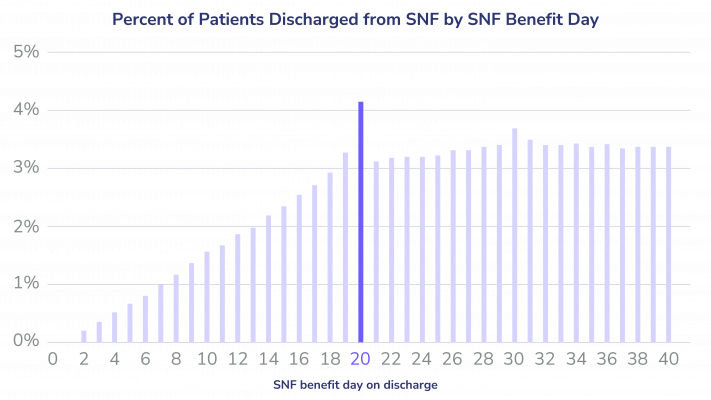
Medicare Advantage (MA) plans tend to use financial incentives and alternative care options to shorten SNF stays, which doesn’t correlate to worse outcomes for patients.4 Traditional Medicare does not generally involve the same degree of active management of SNF utilization or length of stay. This can lead to longer stays, especially when facilities take advantage of the system.5
Accountable Care Organizations (ACOs) represent a path to managing skilled nursing facility (SNF) care for traditional Medicare patients with the same efficiency as Medicare Advantage (MA) plans, which could generate substantial savings. Let’s break down the numbers:
- MA patients typically experience 20–30% shorter SNF stays, which means a reduction of 4–5 days per patient.
- With an average cost of $550 per day for SNF care, that adds up to a saving of $2,475 per patient.
- Since ~1.5 million traditional Medicare beneficiaries use SNFs each year, this approach could save up to $4 billion annually ($40 billion over 10 years).
Other efficiencies, like lowering hospital readmissions and moving care to more affordable home health services, could lead to even bigger cost reductions without sacrificing patient outcomes.
The greatest contribution to overall financial efficiency involves minimizing hospital readmissions. Existing evidence, looking at the high volume episode of hip surgery, suggests that SNFs with high quality metrics deliver reduced readmissions, regardless of the median length-of-stay.6 These studies collectively suggest that healthcare systems should prioritize enhancing the quality of SNF care delivery — including better care coordination, appropriate staffing levels, and evidence-based clinical protocols — rather than extending lengths of stay as a strategy to reduce hospital readmissions.
How to Reduce Unnecessary Stays and Protect Patients
To reduce unnecessary stays, policymakers, regulators, and healthcare leaders must take decisive action. We are calling on CMS to reassess payment models to discourage this behaviour and to bolster efforts to help us improve quality, care models, and cost in the best interest of patients and all Medicare beneficiaries. Key reforms include:
1. Stricter Oversight and Fraud Detection
CMS and the Department of Justice must continue expanding audits and penalties for SNFs engaging in fraudulent billing. Recent fraud settlements have exposed major corporate abuse, but more proactive enforcement is needed in traditional Medicare.
2. Greater Transparency in Discharge Planning
Patients and families must be clearly informed of their right to choose home-based care alternatives instead of prolonged SNF stays, where applicable. Healthcare providers should focus on early discharge planning, rather than defaulting to extended institutionalization.
3. Expansion of Home-Based Care Options
Many patients do not need a SNF stay at all. Programs such as the SNF-at-Home model, expanded home health services, and Hospital-at-Home programs can reduce unnecessary SNF utilization while improving recovery outcomes. CMS should explore greater reimbursement flexibility for these alternatives.
4. Aligning Financial Incentives with Patient Outcomes
Instead of reimbursing SNFs based on length of stay, Medicare should:
- Tie payments more directly to functional improvement and patient recovery
- Implement stricter length-of-stay caps based on clinical benchmarks
- Reward facilities that successfully transition patients home faster with lower readmission rates
Conclusion: Reducing Overstays and Putting Patients First
Improving SNF care isn't just about cutting costs — it's about designing a system that rewards quality outcomes and empowers patients.
Accountable care organizations are incentivized to keep their patients healthy while reducing costs, which has resulted in high quality ACOs achieving significant efficiencies relative to unmanaged fee-for-service Medicare. Medicare ACOs also have several tools and waivers available to support better management of SNF utilization.
SNFs play an essential role in post-acute care, but the current reimbursement model allows for abuse, costing taxpayers billions of dollars. By keeping patients in facilities longer than necessary, some SNFs prioritize profit over patient well-being. In order to see true behavior change, we need to move more of the system towards value-based care. CMS should consider implementing incentives for broader adoption of total-cost-of-care risk models in Traditional Medicare and test quality measures oriented around ensuring accountability for SNF length-of-stay.
At Pearl Health, we partner with primary care physicians and a high quality network of SNFs to improve the quality of patient care while simultaneously lowering the total cost of care. If you want to help us on our mission, reach out.
- According to Medicare billing rules, the SNF stay must be preceded by an inpatient stay of at least three days and the reason for the ongoing stay must match the inpatient diagnosis.
- Medicare, “Skilled Nursing Facility Care”.
- Rachel M. Werner, R. Tamara Konetzka, Mingyu Qi, and Norma B. Coe, "The Impact of Medicare Copayments for Skilled Nursing Facilities on Length of Stay, Outcomes, and Costs," Health Services Research 53, no. 6 (2018): 4625–46.
- Mark D. Neuman, Christopher Wirtalla, and Rachel M. Werner, "Association Between Skilled Nursing Facility Quality Indicators and Hospital Readmissions," JAMA. Oct 2014.
- MedPAC, “March 2022 Report to the Congress: Medicare Payment Policy,” Mar 2022.
- Mark D. Neuman, Christopher Wirtalla, and Rachel M. Werner, "Association Between Skilled Nursing Facility Quality Indicators and Hospital Readmissions," JAMA. Oct 2014; Berg-Weger, MarlaHenderson-Kalb, JuliaZubatsky, MaxLundy, Janice et al. “Cognitive Stimulation Therapy: A Tool for Your Practice With Persons With Dementia?” Journal of the American Medical Directors Association.





