Financial, operational, and clinical results—delivered through smarter strategy and tech-enabled care.
Pearl enables health systems to unlock margin, strengthen care delivery, and improve performance—through aligned risk partnerships, AI-enabled technology, or both.
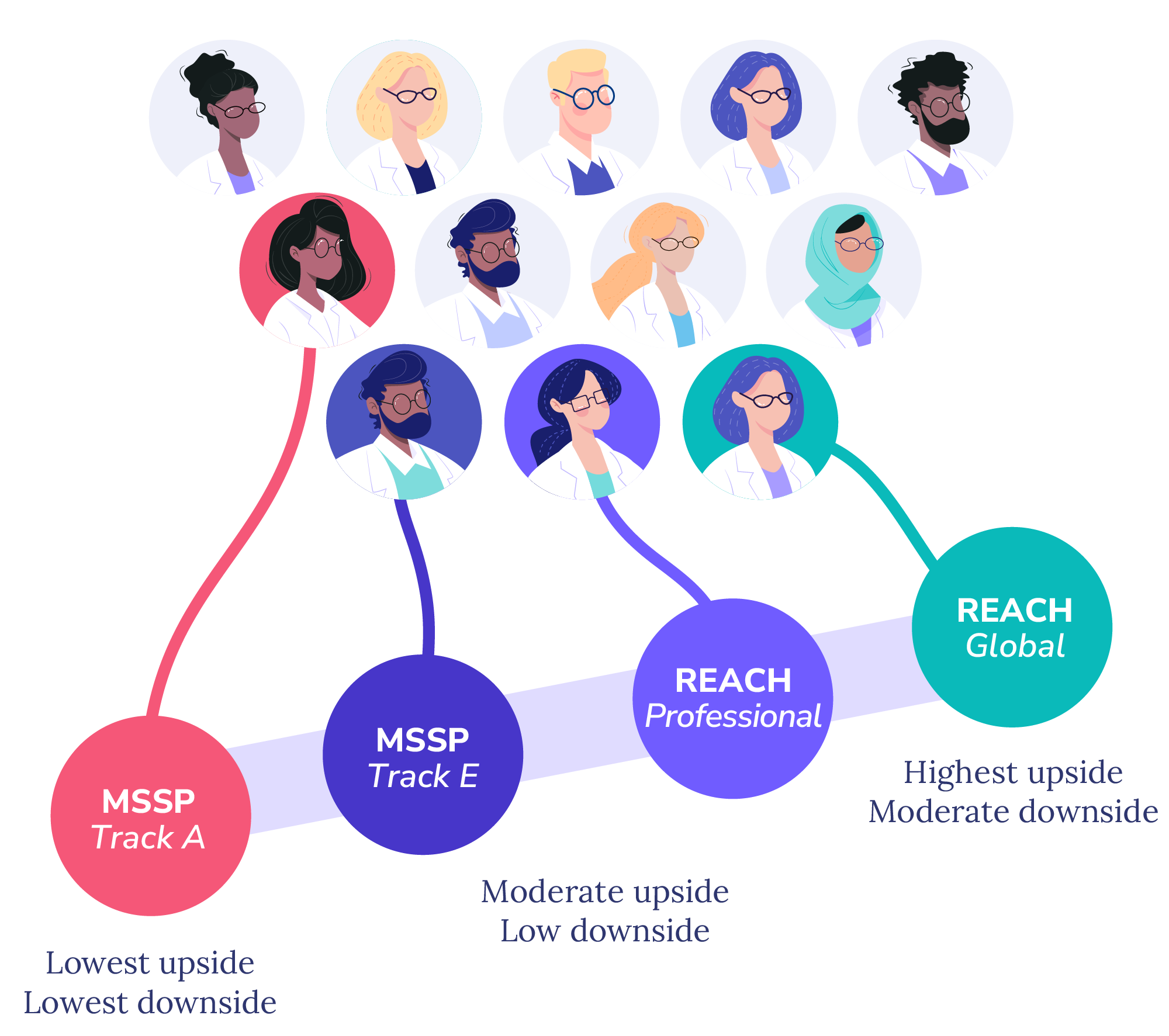
Align providers with Medicare models that fit their readiness and performance potential.
We use actuarial modeling and predictive analytics to match providers with the Medicare arrangements that fit their readiness and potential—designing portfolios that maximize savings, reduce unnecessary risk, and unlock new revenue opportunities.
Ensure top performers capture the full value of their results.
Our incentive structure rewards performance directly and predictably. Transparent distribution rules ensure top performers capture the full value of their results, building accountability and trust.


Turn patient signals into automated, workflow-integrated actions that reduce burden and prevent avoidable costs.
Pearl’s platform surfaces patients with the highest opportunity for impact, ranks them by urgency, automates next steps, and integrates into existing EHR workflows. This reduces administrative burden and enables care teams to focus more time on patients.
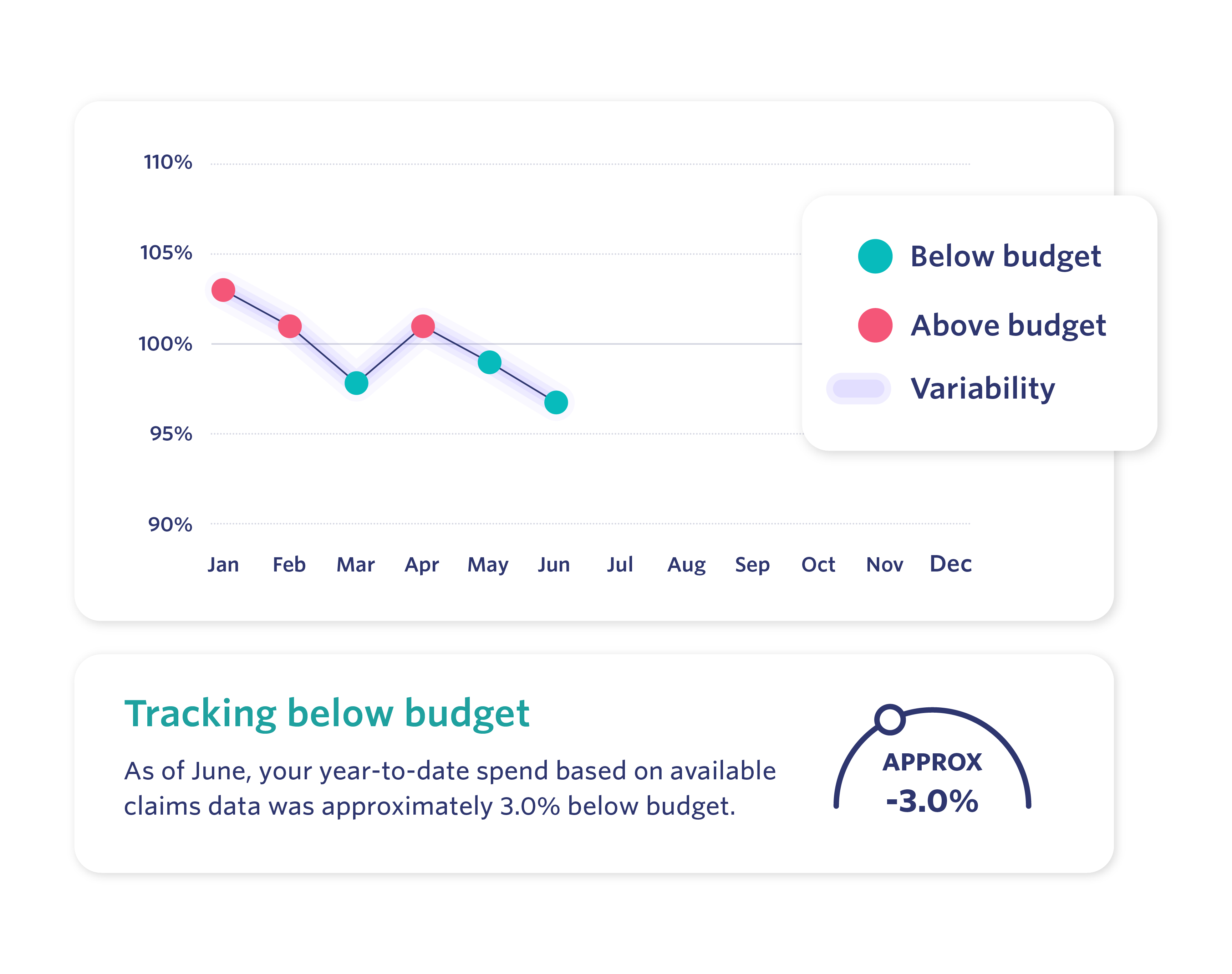
Transform complex data into role-specific priorities, goals, and tracking to align leaders and teams.
Pearl distills complex data into context-aware, role-specific guidance. Leaders gain clear priorities, measurable goals, and real-time tracking, while care teams receive direction tailored to their responsibilities—creating alignment around the actions that drive clinical and financial success.


As Medicare patient volumes grow and fee-for-service economics erode, health systems struggle to maintain margin. Demographic shifts and evolving reimbursement models demand smarter strategies for optimizing revenue while continuing to deliver high-quality, cost-effective care.


Many health systems default to placing all providers and affiliates in the same payment model—regardless of readiness or performance potential. This limits participation, suppresses savings, and leaves value on the table. A more strategic, portfolio-based approach can optimize outcomes across diverse provider cohorts.


Most population health and care coordination teams lack the predictive insights needed to identify at-risk patients before problems escalate. Without data-driven guidance on where to focus their efforts, teams remain stuck in reactive workflows that limit impact.
























Request a complimentary analysis to discover how much value Pearl can unlock in your Medicare portfolio.
