Health Maintenance Organizations (HMOs) managed the care of over 95 million Americans in 2018. These entities are legal insurance organizations characterized by shared technology across providers, cost reduction measures (prior authorization and referral requirements), and predefined networks.
Under the restricted network model, which make up the majority of existent HMO entities, a network of multi-specialty physician groups, Independent Practice Associations, and independent providers contract with an HMO. Beneficiaries enrolled in an HMO plan are required to see a provider within their predefined network, unless they subscribe to a plan with a Point-of-Service (POS) option.
Similar to the Direct Contracting Model, Medicare HMO plans task primary care providers with managing the care of their Medicare patients. The PCP has discretion to grant referrals to specialists in the network, order tests, and steer the ultimate direction of care for their patients. Academics call this role “gatekeeping” because the provider is the ultimate decision maker when it comes to accessing specialist care: patients who sidestep referral requirements by going out of network are faced with the full cost of care – an option that is not financially feasible for most.
What’s classified as “sidestepping” is not always obvious. When a patient makes a visit to an emergency room, they are risking a costly bill in their mail that HMOs will only partially cover. HMO plan administrators make the rules about what is classified as an emergency. The delineation of what is considered a “life-threatening emergency” versus “non-life threatening” is muddied by convoluted layers of insurance jargon. When a patient is experiencing what they believe to be a medical emergency, they generally do not have the time nor the medical expertise to determine whether their medical episode is life-threatening or not. Ultimately, HMOs can create a confusing experience for the patient while disincentivizing them from prioritizing their health.
Direct Contracting is therefore likely a better alternative for Medicare patients looking to avoid these dynamics, as Direct Contracting Entities (DCEs) take a more holistic approach to patient care. Under the DC model, instead of acting as a gatekeeper of specialist care, PCPs instead are able to direct a patient’s care journey while prioritizing long-term health and cost containment. Rather than denying coverage for unmanaged care, DCEs incentivize patients to visit “preferred providers” by keeping costs low for those visits. For instance, beneficiaries being treated by providers working with Pearl will experience reduced or waived copays for going to a preferred provider that their PCP refers them to. Additionally, providers are incentivized to maintain lower total cost of care on beneficiaries which means they spend more time on proactive care to prevent emergency room visits in the first place. However, when emergencies happen, as they inevitably will, Medicare beneficiaries aligned to a DCE have the same open access privileges as any Traditional Medicare beneficiary, meaning their emergency care will be covered and they won’t be punished for looking out for their health.
The advantages that HMOs offer to both the provider and patient are not unique to the HMO model. Since both HMOs and DCEs share the underlying framework of defined networks and centralized care management, they share certain advantages. Both models are conducive to shared technology, which further aids the coordination of patient care across referrals, from PCP to specialist. Further, both models result in an overall lower cost of care as plan administrators have the ability to negotiate with certain providers to keep prices low, in exchange for directed patient traffic.
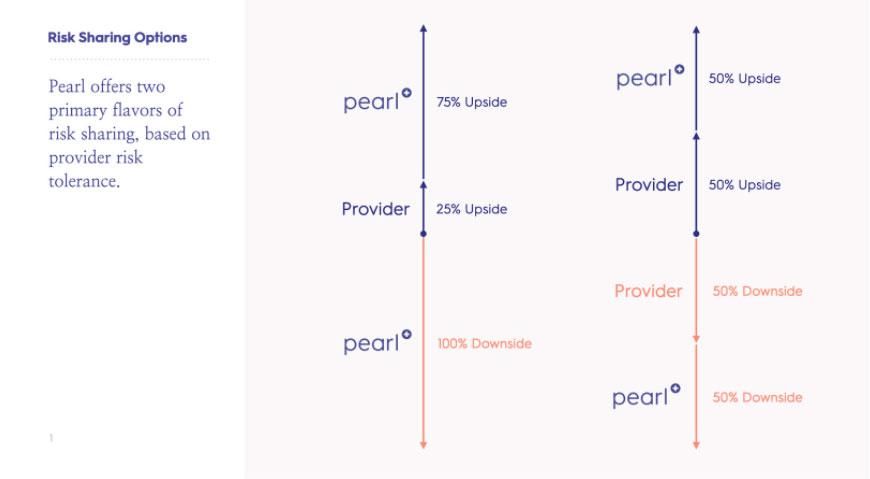
For providers, the capitated payments and risk sharing components of Direct Contracting allow for a more diverse set of financial risk arrangements. For example, Pearl allows participating providers to choose among a number of risk sharing options that vary by downside and upside risk. These options can change year to year as doctors become more comfortable managing their beneficiaries’ care under this new model. Doctors who are effectively able to maintain the health of their patient population while keeping costs below risk-adjusted benchmarks will share in the cost-savings. Furthermore, through standardized quality measures, Pearl ensures that cost saving does not come at the expense of high-quality patient care.
One issue that HMO organizations struggle to curtail is the administrative costs associated with managing patient care. According to a study published in Annals of Internal Medicine, administrative costs in the US amount to 34% of total health care spending. Direct Contracting Entities, such as Pearl, are better situated in this respect: DCEs do not need to manage claims adjudication or conduct utilization review or prior authorizations, substantial components of HMO operations. Pearl aims to maximize the health of our patients, which means directing our spending where it matters most: patient care.
Ultimately, under the HMO model, patient autonomy and service coverage are limited by narrow networks and referral requirements. These conditions, though meant to keep costs low, can result in a confusing experience for not only patients but providers as well. The DC model capitalizes on the advantages of HMOs, such as shared technology across the network and coordinated PCP-focused care, while still enabling both physicians and their beneficiaries to have greater control over the direction of patient care. Rather than punishing beneficiaries for accessing care outside their network, DCEs reward beneficiaries for following the care protocols defined by their PCP.